Weight loss is often seen as a simple equation: burn more calories than you consume. But in reality, your body can fight against your efforts in subtle ways, including through medications you take every day. Some prescribed drugs may interfere with metabolism, appetite, or water retention, making it harder to shed those extra kilos. Understanding these hidden obstacles is crucial for anyone committed to losing weight naturally. Below, we explore 10 common medications that may sabotage your weight loss efforts and how to approach your journey safely, according to health experts.
1. Antidepressants
Many people rely on antidepressants to manage mental health conditions, but some of these medications can increase appetite or slow metabolism. Dr. Carrié, a nutritionist, notes that “certain selective serotonin reuptake inhibitors (SSRIs) may cause mild weight gain in a few weeks or months, even when diet and exercise remain unchanged.” Health experts recommend tracking weight changes and discussing alternatives or adjustments with your prescribing doctor if unwanted weight gain occurs. Balancing mental health and weight loss requires careful monitoring rather than abrupt discontinuation of therapy.
2. Corticosteroids
Corticosteroids, such as prednisone, are widely prescribed for inflammation or autoimmune conditions. Experts point out that these medications can lead to fluid retention, fat redistribution, and increased appetite. According to nutritionist Dr. Carrié, “patients on long-term corticosteroids often report unexpected weight gain around the abdomen, face, and neck.” While necessary for medical conditions, it’s important to pair corticosteroid use with a controlled diet and exercise plan to minimize weight gain.

3. Antihypertensives
Blood pressure medications like beta-blockers and certain calcium channel blockers may slow your metabolism or reduce energy levels, making physical activity more challenging. Cardiologist Dr. Léa Durand explains, “Patients sometimes notice modest weight gain on beta-blockers, though the benefits for heart health outweigh the risks. Awareness helps in adjusting lifestyle factors like diet and exercise.” Choosing the right antihypertensive or adjusting timing and dosage can reduce their impact on weight.

4. Antipsychotics
Second-generation antipsychotics are crucial for managing conditions such as schizophrenia or bipolar disorder. However, experts caution that they often increase appetite, promote insulin resistance, and alter fat storage. Dr. Carrié adds, “Weight gain on antipsychotics can be significant over months. Nutritional support, monitoring, and low-calorie, protein-rich meals help patients maintain a healthier balance.” For those on these medications, combining natural, nutrient-dense foods with regular activity is essential.
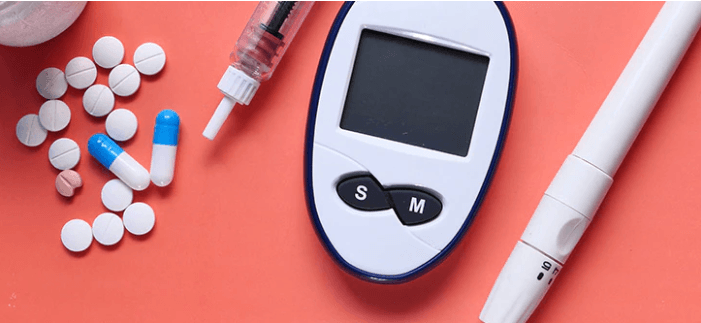
5. Diabetes Medications
Ironically, some drugs used to treat diabetes, like insulin or sulfonylureas, may contribute to weight gain. Endocrinologist Dr. Julien Renaud says, “While these medications help control blood sugar, they can also increase fat storage if caloric intake isn’t adjusted accordingly.” Experts recommend combining blood sugar management with high-fiber, low-glycemic foods and regular physical activity to reduce the risk of gaining weight while maintaining glycemic control.
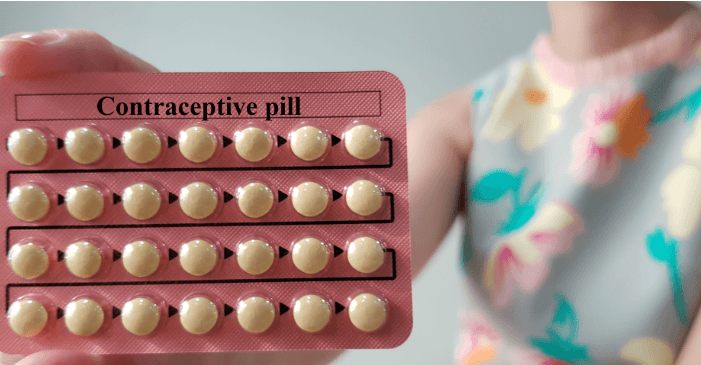
6. Hormonal Contraceptives
Oral contraceptives, patches, and hormonal IUDs are widely used, but some may slightly increase fluid retention or appetite. Dr. Carrié explains, “Not all hormonal contraceptives cause weight gain, but certain formulations can lead to minor increases, especially in the first months of use.” Maintaining a nutrient-rich diet, drinking plenty of water, and monitoring body composition rather than just scale weight can help mitigate these effects.
7. Anti-seizure Medications
Certain anti-seizure medications prescribed for epilepsy or neuropathic pain may promote weight gain. Neurologist Dr. Sophie Garnier notes, “Medications like valproate or carbamazepine can increase appetite and lead to fat accumulation.” Experts advise patients to track caloric intake, focus on lean proteins and vegetables, and engage in moderate exercise to counteract these side effects.
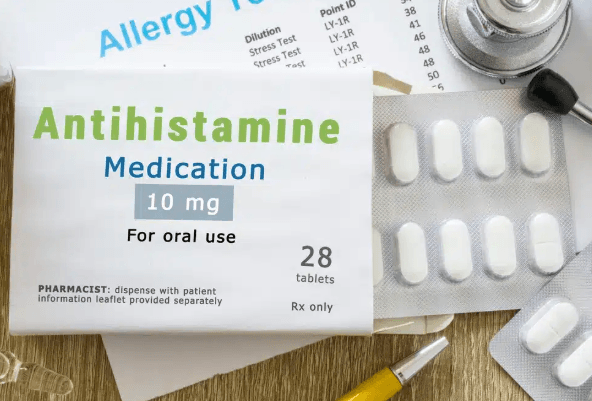
8. Antihistamines
Over-the-counter antihistamines for allergies are convenient but may have a subtle effect on weight. Dr. Carrié explains, “Some first-generation antihistamines cause drowsiness, reduce activity, and may slightly increase appetite, leading to gradual weight gain.” Choosing non-drowsy alternatives and maintaining regular physical activity can help prevent weight changes while managing allergies.
9. Proton Pump Inhibitors (PPIs)
PPIs, used to manage acid reflux or ulcers, can alter gut microbiota and reduce nutrient absorption. While the weight gain effect is not dramatic, Dr. Carrié points out that “long-term PPI use may subtly affect metabolism or appetite regulation, making it slightly harder to lose weight naturally.” Pairing these medications with a fiber-rich diet and regular exercise helps maintain digestive health and support weight management.

10. Beta-2 Agonists
Medications for asthma or COPD, like albuterol, may trigger temporary fluid retention or increase appetite in some patients. Pulmonologist Dr. Marc Lefèvre notes, “Although essential for respiratory health, some patients notice weight fluctuations when using these inhalers. Ensuring proper nutrition and exercise helps offset minor weight changes.” Consulting your healthcare provider about timing and dosage can help minimize any impact on weight loss goals.