Suicide is a complex public health issue influenced by psychological, social, and medical factors. Certain health conditions increase the risk significantly, and understanding them can help in early identification and intervention. According to experts, both physical and mental illnesses contribute to heightened vulnerability, especially when combined with stress, social isolation, or substance use. Recognizing these conditions and seeking timely professional help can save lives. Awareness campaigns and regular mental health screenings are critical to reducing suicide rates and ensuring individuals receive support before reaching a crisis point.

1. Major Depressive Disorder
Major depressive disorder is one of the most strongly associated mental health conditions with suicide risk. Individuals experiencing persistent sadness, hopelessness, and a lack of interest in activities may develop thoughts of self-harm. Experts emphasize that depression often goes undiagnosed, particularly in men and older adults, who may express symptoms differently. Early recognition, therapy, and medication can significantly reduce suicide risk. According to Dr. Thomas Joiner, a leading psychologist in suicidology, the severity of depression and the presence of hopelessness are key predictors of suicidal behavior. Prompt intervention is essential.

2. Bipolar Disorder
Bipolar disorder, characterized by extreme mood swings, significantly increases suicide risk. During depressive episodes, individuals may experience intense despair, while manic or mixed states can trigger impulsivity. Research suggests that nearly one in three people with bipolar disorder attempt suicide in their lifetime. Mental health professionals recommend mood stabilizers, psychotherapy, and close monitoring as essential measures. Family and community support are also crucial. According to the National Institute of Mental Health, early diagnosis and consistent treatment reduce the likelihood of self-harm. Awareness of warning signs can prevent tragic outcomes.

3. Schizophrenia
Schizophrenia, a severe psychiatric disorder involving hallucinations, delusions, and cognitive impairment, carries a high suicide risk. Experts note that about 5-10% of individuals with schizophrenia die by suicide. Feelings of isolation, stigma, and distorted reality contribute to suicidal thoughts. Antipsychotic medications, therapy, and social support systems are vital for risk reduction. According to Professor Anthony Morrison, social integration and adherence to treatment plans are among the strongest protective factors. Educating caregivers and families on early warning signs is also crucial for intervention.
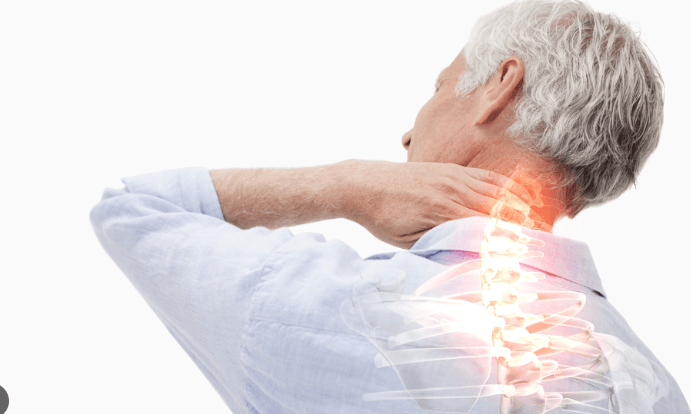
4. Chronic Pain Conditions
Chronic pain, including back pain, arthritis, and fibromyalgia, can increase suicide risk due to prolonged suffering and reduced quality of life. Pain often leads to sleep disturbances, anxiety, and depression, compounding the risk. Dr. Harold Rogers, a pain management specialist, explains that multidisciplinary approaches—including medication, physical therapy, and counseling—help mitigate mental health consequences. Awareness of the psychological impact of chronic pain is essential. Patients should be encouraged to discuss emotional distress with healthcare providers, as integrated care reduces the likelihood of suicidal ideation.
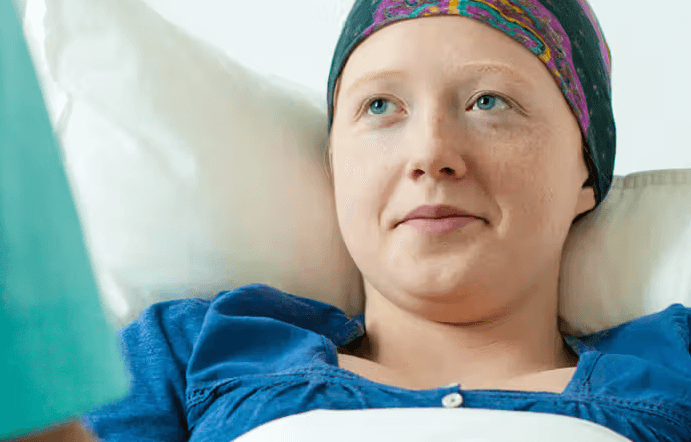
5. Cancer
Cancer patients face a heightened suicide risk, particularly during diagnosis and treatment periods. The physical and emotional toll, along with fears about prognosis and treatment side effects, can lead to depression and hopelessness. Oncologists and mental health professionals recommend early psychological support and counseling. Studies show that access to palliative care, support groups, and therapy significantly reduces suicide risk. Professor Susan Folkman, an expert in psycho-oncology, emphasizes that open communication about mental health is essential. Support networks and professional guidance provide patients with coping strategies and hope.
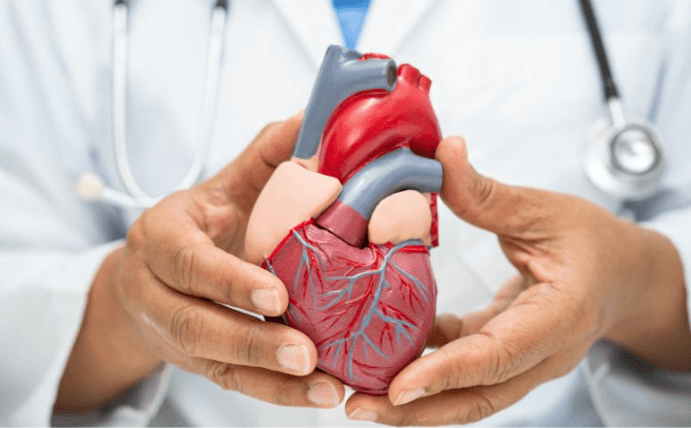
6. Cardiovascular Diseases
Heart disease and stroke are linked to increased suicide risk, especially in individuals experiencing functional limitations or chronic illness-related stress. Depression often co-occurs with cardiovascular conditions, intensifying vulnerability. Experts recommend screening for depression in patients with chronic heart conditions. Dr. Naomi Simon, a cardiologist specializing in psychosomatic medicine, notes that lifestyle interventions, therapy, and medication management can help reduce risk. Awareness of warning signs, including withdrawal and mood changes, is key to prevention. Collaboration between cardiologists and mental health professionals improves outcomes.
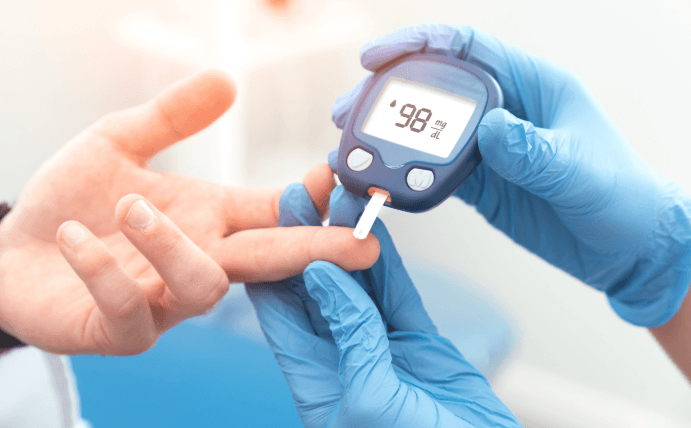
7. Diabetes
Diabetes management involves constant attention to diet, medication, and blood sugar monitoring, which can cause stress, anxiety, and depression. Research indicates that people with diabetes, particularly type 1, face higher rates of suicidal thoughts and attempts. Mental health screenings and counseling integrated into diabetes care are essential. Dr. Ellen B. Goldstein highlights that support from healthcare providers and peer groups significantly lowers risk. Encouraging patients to discuss emotional struggles openly ensures timely intervention. Diabetes self-management programs that include mental health components show promising results in suicide prevention.

8. Substance Use Disorders
Substance use disorders—including alcohol, opioids, and stimulants—are strongly linked to suicide risk. Impulsivity, depression, and social isolation often accompany addiction, compounding vulnerability. According to the Substance Abuse and Mental Health Services Administration (SAMHSA), integrated treatment addressing both substance use and mental health significantly reduces suicidal behavior. Behavioral therapy, medical supervision, and social support are key elements. Early identification and intervention are critical, as relapse or withdrawal periods may heighten risk. Professionals stress that understanding addiction as a medical condition helps reduce stigma and encourage treatment-seeking.

9. Neurodegenerative Diseases
Neurodegenerative conditions like Parkinson’s and Alzheimer’s disease can increase suicide risk due to progressive loss of independence, cognitive decline, and depression. Early psychological support and counseling are vital. Dr. Linda Clare, a specialist in neuropsychology, emphasizes that caregiver education and structured daily routines help reduce stress and isolation. Patients benefit from therapy, medication, and social engagement. Awareness of mood changes, agitation, and hopelessness allows timely intervention. Multidisciplinary care teams improve patient quality of life and reduce the likelihood of suicidal thoughts.

10. HIV/AIDS
Individuals living with HIV/AIDS face both physical and psychosocial stressors that heighten suicide risk. Stigma, chronic illness management, and concerns about prognosis can trigger depression and hopelessness. Studies show that access to mental health services, antiretroviral therapy, and social support networks reduces suicidal behavior. Dr. Robert Remien, an expert in HIV psychology, stresses that open communication with healthcare providers and peer support is essential. Comprehensive care addressing both physical and mental health needs is the most effective strategy for reducing suicide risk among HIV-positive individuals.



